Effects of Weight-Bearing Exercise on Health-Related Physical Fitness and Sleep Indicators in Pre- and Postmenopausal Women
Article information
Trans Abstract
PURPOSE
This study aimed to determine the effects of weight-bearing exercise on health-related physical fitness and sleep index in pre- and postmenopausal women.
METHODS
Twenty middle-aged women were randomly assigned to premenopausal women (PRW; n=11) and postmenopausal women (POW; n=9) groups. All subjects engaged in weight-bearing exercises for 50 minute twice a week for 8 weeks. All participants underwent weight, body mass index (BMI), muscle mass (MM), body fat mass, body fat percentage, waist to hip ratio, bench press (BP), leg press (LP), 3-minute step test (3 MST), sit and reach test (SRT), air squat (AS), push up (PU), curl up (CU), grip strength (GS), and the Korean version of the Pittsburgh Sleep Quality Index (K-PSQI) measurements before and 4 and 8 weeks after the weight-bearing exercise program.
RESULTS
AS and PU improved significantly in the PRW versus POW group (p<.05). BP, LP, 3MST, SRT, AS, PU, CU, GS, and K-PSQI improved significantly in the PRW and POW groups (p<.05).
CONCLUSIONS
Weight-bearing exercise improved health-related fitness and sleep indicators in pre- and postmenopausal women. In particular, weight-bearing exercises more effectively improved the muscle endurance of pre- versus postmenopausal women. This significant finding suggests that the fitness level and sleep quality of premenopausal women may benefit from regular weight-bearing exercise.
INTRODUCTION
Menopause is a condition in which a woman's ovarian function de-clines with age and normal menstruation ceases [1]. Postmenopausal symptoms include hot flushes, excessive body heat, and sweating caused by estrogen [2]. Weight gain is an important problem after menopause [3], and it has been reported that the increase in body shape and abdom-inal fat to compensate for the decrease in estrogen after menopause [4] causes metabolic syndrome [5] and vascular disease [6]. Postmenopausal women's health-related physical fitness, such as physical strength, muscle strength, and muscular endurance, deteriorate due to endocrine system deterioration, and a decrease in physical activity after menopause leads to musculoskeletal disorders [7]. Furthermore, postmenopausal women suffer from sleep disorders such as insomnia, sleep-related breathing disorders, and sleep disruption due to hormonal changes [8]. Postmenopausal women experience fatigue and deprivation as a result of sleep disruption, which leads to psychological disorders and exacerbates sleep disorders [9]. As such, menopause is a natural phenomenon caused by aging, but it is also a time when various diseases are induced [10], and it has been reported that the symptoms of menopause affect the quality of life [11]. Kang [12] argued that as the average lifespan increases, so does the importance of living a healthy life after menopause. Regular exercise has been shown to improve the physical and psychological health of postmenopausal women, exercise is necessary to alleviate stress, enhance quality of life, and get enough sleep due to physical changes after menopause [13]. However, while exercise is associated with a reduction in body weight, body mass index (BMI), and vascular disorders in postmenopausal women [6], another study claims that exercise results in postmenopausal women are insignificant [14]. Therefore, it is necessary to investigate the effects of exercise in both premenopausal women and postmenopausal women in order to reduce postmenopausal symptoms and problems.
Dance sports [15], Pilates [16], yoga [17], and resistance exercise [18] are all exercises that improve the physical health of postmenopausal women. Resistance exercise is a muscle-strengthening exercise that contracts and relaxes muscles within the range of motion of the joint, and it has been reported to improve muscle strength and physical fitness in Postmenopausal women [18]. Notably, weight-bearing exercise (WBE) is a type of resistance exercise. WBE is an exercise that uses one's own body weight to increase muscle strength and endurance, and it has the advantage of allowing the exercise intensity to be adjusted based on one's physical ability [19]. Moreover, WBE is used to improve motor function in subjects with low physical fitness [20], and it has been shown to be effective in improving muscle strength and preventing muscle aging [21]. However, the majority of studies on WBE in postmenopausal women have fo-cused on bone density [22], with few studies examining the effects on health-related physical fitness, such as body composition, muscle strength, and muscular endurance.
Therefore, the purpose of this study is to compare and review the effects of WBE on health-related fitness and sleep indicators in middle-aged women by categorizing them as premenopausal or postmenopausal. We hypothesized that WBE would improve health-related health and sleep indicators significantly more in premenopausal women than in postmenopausal women.
METHODS
1. Participants
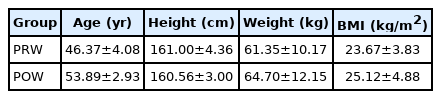
This study women from Gyeonggi-do in South Korea were recruited and randomly divided into two groups: premenopausal women (PRW, n=11) and postmenopausal women (POW, n=9). All participants had sufficient understanding of the experiment and agreed to participate by signing documents detailing the scope and procedures of the experiment and the academic use of the results beforehand. The criteria for in-clusion of participants were middle-aged white-collar women who had no experience in resistance exercise training for a year and with no or-thopedic, cardiovascular, and psychiatric disorders before. Additionally, they did not engage in many hobbies and were most active at night after work. The criteria for subjects in the postmenopausal women group were those who had been menopausal for 12 months or more [1]. The physical characteristics of the subjects are shown in Table 1.
2. Experimental design
Body composition, 1RM muscle strength, and physical fitness were measured as health-related physical factors, and the condition of sleeping was evaluated using the Pittsburgh sleep quality index. All measurements were taken before the start of WBE and after 4 and 8 weeks of exercise, respectively. The WBE included 5 minutes of warm-up, 40 minutes of weight-bearing exercise, and 5 minutes of cool-down. All subjects engaged in WBE for 50 minutes per day, twice a week, and for 8 weeks.
3. Measurement
1) Health-related physical fitness
Body composition, 1RM muscle strength, and physical fitness for the health-related fitness index were measured before, 4 weeks, and 8 weeks after WBE, respectively.
Body composition was measured for each body part using a body composition measuring instrument (Inbody 330, Biospace, Korea) based on the bioelectrical impedance method, which is a method of measuring impedance for each body part using multi-frequency analysis. Weight, muscle mass (MM), body fat mass (BFM), and body fat percentage (BFP) were all measured, and the body mass index (BMI) and waist to hip ratio (WHR) were calculated. The subject wiped the palms and soles of her feet with an electrolyte tissue and placed them on both power electrodes. The measurements were taken while holding both hand electrodes and keeping the arms and armpits 30 degrees apart to prevent them from touching [23]. To minimize measurement error, meals, beverages, alcohol, and other beverages, as well as vigorous physical activity, were re-stricted 2 hours before measurement.
The 1RM muscle strength of the pectoralis major muscle was measured using a bench press, and the muscle strength of the quadriceps femoris was measured using a leg press. The subjects did aerobic exercise and dynamic stretching for 10 minutes, then rested for 1 minute after 5 to 10 repetitions with a light weight. The exercise was repeated until the subject could repeat the maximum number of repetitions, and if the number of repetitions was 10 or more, the exercise was rested for 3 minutes. The weight was then increased, and the weight and number of repetitions performed less than 10 times were measured and entered into the indirect estimation equation. The indirect estimation formula used 1RM=lifted weight+(lifted weight×number of lifts×0.025) [24].
Physical fitness consists of a 3-minute step test (3 MST), a sit and reach test (SRT), an air squat (AS), a push up (PU), a curl up (CU), and grip strength (GS) were used to assess [23]. 3 MST is a cardiorespiratory endurance test in which the subject climbed up and down the step box for 3 minutes to the sound of a 96-bit metronome, then palpated the nodules within 5 seconds and measured the heart rate for 60 seconds. SRT measures flexibility by having the subject sit with both feet on the vertical plane of the measuring device, extend the knee, and measure how far their upper body bends forward. The highest value among the three repeated measurements for SRT was chosen as the measured value. AS was a test of the muscular stamina of the lower body. It counts the number of times the subject made the repeated 90-degree bends and ex-tensions to prevent their knees from extending past their toes while standing with their legs shoulder-width apart for one quarter. PU was used to assess upper body muscular endurance, and the subject was placed in a prone position with knees on the floor and arms extended. The number of times the elbows were bent and extended to 90 or less accurately repeated at the fastest possible speed for 1 minute while keeping the shoulders and hips level was counted. CU are used to assess ab-dominal muscular endurance and were measured on a mat with two tapes attached at 10 cm intervals. The movement of raising and lowering the upper body by about 30 degrees with the tips of both hands on the tape after bending the knees by 90 degrees while lying on the mat was accurately repeated as fast as possible for 1 minute. GS was a measure of overall strength, and it was measured using a dynamometer (EH-101, CAMRY, China). In a standing position, subjects were measured by holding a manometer so that the second joint of the finger was at a right angle and the arm was spread out about 15 degrees. The highest value was used as the measured value after repeated measurements of the right and left hands with the maximum pressure in order [25].
2) Sleep
The Korean version of the Pittsburgh sleep quality index (K-PSQI) was measured before, 4 weeks, and 8 weeks after WBE. The K-PSQI consists of seven items: subjective sleep quality, sleep latency, sleep duration, habitual sleep efficiency, sleep disturbance, use of sleep medication, and daytime dysfunction. Scores are assigned on a scale of 0 to 3, with a maximum score of 21. The higher the score, the lower the quality of sleep, and the closer the score was to 0, the better the quality of sleep [26].
4. Weight bearing exercise
WBE was performed for a total of 50 minutes in this study, as shown in Fig. 1 and Table 2, with 5 minutes of warm-up exercise, 40 minutes of main exercise, and 5 minutes of cool-down exercise. WBE was performed between 6 and 7 p.m., taking into account the subject characteristics of middle-aged white-collar women, and in an environment with an indoor temperature of 15-20° and a humidity of 40-60%. WBE was performed by two exercise specialists who majored in sports science, and the exercise intensity was 1RM 30% (1 week: 1 set of 15 reps, 2-4 weeks: 2 sets of 15 reps, 5-8 weeks: 2 sets of 20 reps), 30 seconds of rest between sets, and 60 seconds of rest between exercises.
5. Statistical analysis
The data were analyzed statistically using SPSS 20.0 software (SPSS, Chicago, IL, USA). An independent sample t-test was used to assess the general characteristics of the subjects. Two-way ANOVA with repeated measures was performed to verify the difference between groups and time periods. A Scheffe post hoc test was used if there was a significant difference between groups and time periods. Statistical significance was reached when p <.05.
RESULTS
1. Health-related physical fitness
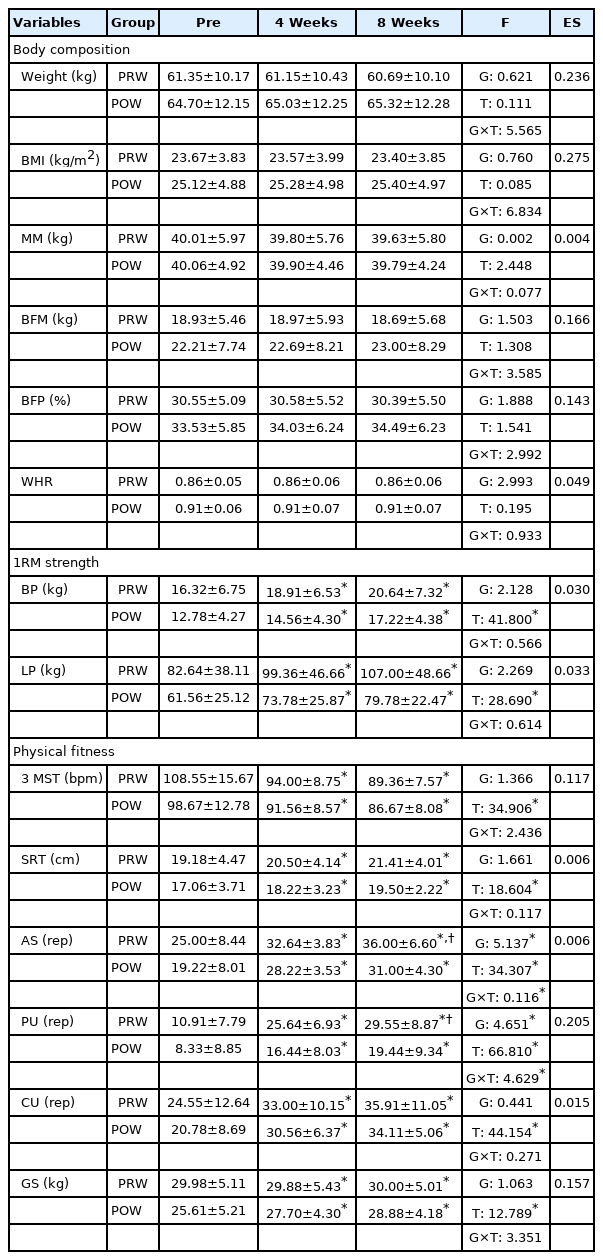
The changes in health-related physical fitness indicators are shown in Table 3. Weight, BMI, MM, BFM, BFP, and WHR for body composition did not statistically significantly interact with groups or periods, but BP and LP for 1RM strength were significantly increased in PRW and POW group after 4 and 8 weeks of WBE, respectively (p <.05). AS and PU for physical fitness improved significantly in the PRW group compared to the POW group (p <.05). 3MST, SRT, AS, PU, CU, and CU were significantly improved in PRW and POW group after 4 and 8 weeks of WBE, respectively (p <.05).
2. Sleep
The changes in sleep indicator is shown in Table 4. K-PSQI was significantly decreased in PRW and POW group after 4 and 8 weeks of exercise, respectively (p <.05).
DISCUSSION
The main finding of this study was that WBE improved health-related fitness and sleep indicators in premenopausal women and Postmenopausal women, with the PRW group performing better than the POW group.
Regular exercise has been shown to help with postmenopausal body changes [13]. Resistance exercise has been shown to improve strength, flexibility, muscular endurance, and cardiorespiratory endurance [27]. WBE, a type of resistance exercise, is effective in improving muscle strength by increasing the size of muscle fibers [21]. Muscular strength, cardiorespiratory endurance, flexibility, muscular endurance, and whole body strength were measured in this study using BP, LP, 3 MST, SRT, AS, PU, CU, and GS. It is thought that muscle strength and physical fitness improved after WBE due to increased muscle activity and muscle fiber. Furthermore, previous research found that age-related hormones such as estrogen and growth hormone secretion were lower in postmenopausal women than in premenopausal women [28]. Estrogen has been shown to increase muscle strength and anabolism [29]. Also, growth hormone has been shown to influence aging rate, muscle mass, bone density, and strength [30]. This study demonstrated an interactive relationship between AS and PU and physical fitness. Particularly, PU demonstrated a large effect size. AS and PU for physical fitness were both higher in PRW group compared to POW group after 4 and 8 weeks of exercise. AS and PU denote lower and upper body muscular endurance, which is thought to be the result of increased muscle strength after WBE due to estrogen secretion in premenopausal women compared to postmenopausal women lacking estrogen. Additionally, AS measures the muscular endurance of the lower body, and when compared to postmenopausal women, premenopausal women have better consistency in exercise and better capacity to sustain movement through muscle activity. Additionally, because PU tests the strength of the upper body muscles, it was determined that premenopausal women had better upper body movement endurance than postmenopausal women in general. Previous research, on the other hand, has found that weight loss without diet control necessitates a lot of exercise [31]. We discovered that the 8 weeks WBE exercise was performed without restricting food intake, which improved muscle strength and physical fitness, but the effect on body composition such as weight and body fat is difficult to predict. This is a topic for future research, and the control of food intake and lifestyle is required. As a result, WBE is effective in improving the health-related physical fitness of women before and after menopause, implying that WBE can be useful as an exercise for preventing estrogen deficiency in premenopausal women and improving muscular endurance.
Disturbance is strongly linked to stress, depression, and anxiety [32], and postmenopausal women have increased tension and fatigue due to hormonal changes [33]. Health-promoting behaviors and exercise have been shown to improve sleep quality in postmenopausal women [34], and resistance exercise has been shown to improve PSQI [35]. However, research on the effect of WBE on sleep in postmenopausal women is limited. K-PSQI was significantly improved in both PRW and POW group after performing WBE for 8 weeks in premenopausal women and postmenopausal women in this study. Sleep is associated with serotonin [36], and serotonin concentration has been linked to physical fitness factors [37]. In other words, sleep disturbance in postmenopausal women may reduce physical fitness due to changes in serotonin concentration. Previous research has suggested that moderate-intensity exercise is required to activate serotonin and improve sleep quality [38]. Regular exercise improved serotonin concentration, sleep time, and sleep latency [39,40], and moderate-intensity exercise was reported to improve sleep time and sleep latency [41]. Additionally, Growth hormone, which is secreted during sleep, is crucial for the body's recovery process, and melatonin, one of the hormones, chemically induces sleepiness and lowers body temperature. So, previous research has suggested that resistance exercise secretes growth hormone and melatonin [42]. According to this study, melatonin and growth hormone are secreted during weight-bearing exercise, which causes postmenopausal women to fall asleep. The results of these previous studies are thought to be the reason why the AS, PU, CU, and GS for physical fitness of premenopausal women and postmenopausal women after WBE improved in this study, that also affected K-PSQI. We thought that in this study, premenopausal women and postmenopausal women improved their physical fitness after WBE, and their hormones are secreted, which improved their sleep quality. Thus, it is considered that regular WBE for 8 weeks improved sleep quality through improving physical fitness, serotonin, Growth hormone, and melatonin are secreted.
There are several limitations in our study. The major part of subjects in this study was middle-aged women in white-collar jobs, and it is not unclear whether the results of this study can be applied to middle-aged women in other occupations. And it has a small sample size and short intervention period. So, it is likely that the 2-month intervention is not enough period. Additionally, it might be better to be investigated the de-mographic characteristics because the subject characteristics of this study did not collect information on pain, alcohol consumption, and medical history. Another limitation is that sleep quality is evaluated only by subjective questionnaire. Finally, there was no follow-up study on af-tereffect of exercise after the end of the intervention.
CONCLUSION
Health-related fitness and sleep indicators were found to be significantly improved in both premenopausal women and postmenopausal women. Muscle endurance of health-related fitness was significantly improved in premenopausal women after WBE compared to Postmenopausal women, suggesting that regular weight-bearing exercise can improve potential health-related fitness and sleep not only after but also before menopause. Future studies should investigate the effect of weight-bearing exercise on physiological and psychological changes in premenopausal women and postmenopausal women based on symptom level.
Notes
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
AUTHOR CONTRIBUTION
Conceptualization: H Lee; Project administration: H Lee; Data curation: W Lee; Formal analysis: J Lee, W Lee, Y Lee; Funding acquisition: W Lee, H Lee; Methodology: J Lee, W Lee, H Lee; Visualization: J Lee, Y Lee; Writing - original draft: J Lee, W Lee; Writing - review & editing: J Lee, H Lee.